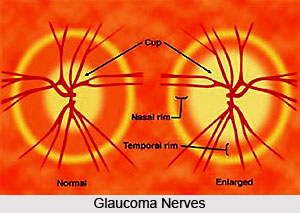
 Several types of Glaucoma like primary glaucoma, pigmentary glaucoma, Exfoliation glaucoma, infantile glaucoma and many others decide the method of treatment. Glaucoma has been classified into specific types.
Several types of Glaucoma like primary glaucoma, pigmentary glaucoma, Exfoliation glaucoma, infantile glaucoma and many others decide the method of treatment. Glaucoma has been classified into specific types.
The first type of Glaucoma is primary glaucoma, which is again classified into primary open-angle glaucoma, also known as chronic open-angle glaucoma, chronic simple glaucoma, glaucoma simplex; low-tension glaucoma, primary angle-closure glaucoma, also known as primary closed-angle glaucoma, narrow-angle glaucoma, pupil-block glaucoma, acute congestive glaucoma; acute angle-closure glaucoma; chronic angle-closure glaucoma; intermittent angle-closure glaucoma and superimposed chronic open-angle closure glaucoma. Pigmentary glaucoma, exfoliation glaucoma, also known as pseudoexfoliative glaucoma or glaucoma capsulare is the two variants of primary glaucoma.
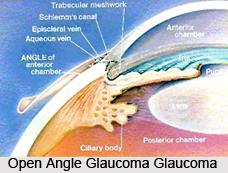
Primary open-angle glaucoma is caused by trabecular blockage, which is where the aqueous humor in the eye drains out. Because the microscopic passage-ways are blocked, the pressure is created in the eye and causes imperceptible very gradual vision loss. Peripheral vision is affected first but gradually the entire vision will be lost if not treated properly. Looking for cupping of the optic nerve is the first step of diagnosis. The goal of the treatment is to release the fluid by opening uveoscleral passageways, which are acted upon by prostoglandin agonists. Beta-blockers such as timolol, work by decreasing aqueous formation. Carbonic anhydrase inhibitors decrease bicarbonate formation from ciliary processes in the eye, thus diminishing the formation of aqueous humor. Parasympathetic analogs are drugs that work on the trabecular outflow by opening up the passageway and contracting the pupil. Alpha 2 agonists both decrease fluid production and increase drainage.
Primary angle-closure glaucoma is caused by contact between the iris and trabecular meshwork, which in turn checks outflow of the aqueous humor from the eye. This contact between iris and trabecular meshwork (TM) may steadily damage the function of the meshwork until it fails to keep the speed with aqueous production, and the pressure rises. In over half of all cases, prolonged contact between iris and TM causes the formation of synechiae. These cause permanent obstruction of aqueous outflow. In some cases, pressure may rapidly build up in the eye thus causing pain and redness. In this situation the vision may become blurred, and halos may be seen around bright lights.
Diagnosis of glaucoma is made from physical signs and symptoms like if the pupils are mid-dilated and unresponsive to light, cornea edematous (cloudy), reduced vision, redness, pain. However, the majority of cases are asymptomatic. Prior to very severe loss of vision, these cases can only be recognised by examination, generally by an eye care professional. Once any symptoms have been controlled, the first line treatment is laser iridotomy. This may be performed using either Nd:YAG or argon lasers, or in some cases by conventional incision surgery. The goal of treatment is to reverse, and prevent, contact between iris and trabecular meshwork. In early to moderately advanced cases, iridotomy is successful in opening the angle in around 75% of cases. In the other 25% laser iridoplasty, medication (pilocarpine) or incisional surgery may be required.
Developmental glaucoma is another type of glaucoma that is categorised into primary congenital glaucoma and infantile glaucoma. Secondary glaucoma is classified into its variants namely Inflammatory Glaucoma, Fuchs Heterochromic Iridocyclitis, Phacogenic glaucoma, Angle-closure glaucoma, Phacoanaphylactic glaucoma, Phacolytic glaucoma, Hyphema and Hemolytic glaucoma, also known as erythroclastic glaucoma. Traumatic glaucoma is another type of glaucoma that usually occurs on anterior chamber angle. Postsurgical glaucoma is classified into Aphakic pupillary block, Ciliary block glaucoma, Neovascular glaucoma, Drug-induced glaucoma, Corticosteroid induced glaucoma and Alpha-chymotrypsin glaucoma.
Neovascular glaucoma is an uncommon type of glaucoma that is almost impossible to treat. This condition is often caused by proliferative diabetic retinopathy (PDR) or central retinal vein occlusion (CRVO). It may also be triggered by other conditions that often result in ischemia of the retina or ciliary body. Patients with poor blood flow to the eye are highly at risk for this condition. Neovascular glaucoma results when new, abnormal vessels begin developing in the angle of the eye that begins blocking the drainage. Patients with such situation begin to lose their eyesight speedily. Sometimes, the disease appears very rapidly, especially after cataract surgery procedure. A new treatment for this disease, as first reported by Kahook and colleagues, involves use of a novel group of medications known as Anti-VEGF agents. These medications through injections can lead to a dramatic decrease in new vessel formation and, if injected early enough in the disease process, may lead to normalization of intraocular pressure.
Toxic glaucoma is open angle glaucoma with significant rise of intraocular pressure following unknown pathogenesis. Intraocular pressure can sometimes reach to about 80 mmHg. It characteristically marks as ciliary body inflammation and are massive trabecular oedema that sometimes extends to Schlemm`s Canal. This condition is distinguished from malignant glaucoma by the presence of a deep and clear anterior chamber and a lack of aqueous misdirection. Also, the corneal appearance is not much hazy. A reduction in visual acuity can occur followed neuroretinal breakdown. Related factors include inflammation, drugs, trauma and intraocular surgery, including cataract surgery and vitrectomy procedures. Some cases of glaucoma can be resolved with some medication, vitrectomy procedures or trabeculectomy. Valving procedures can give some assistance but further research is also required.
Several types of glaucoma exist and with modern advancement in medicine, treatments are also in abundance. However, proper diagnosis is very important to select the appropriate method of treatment.